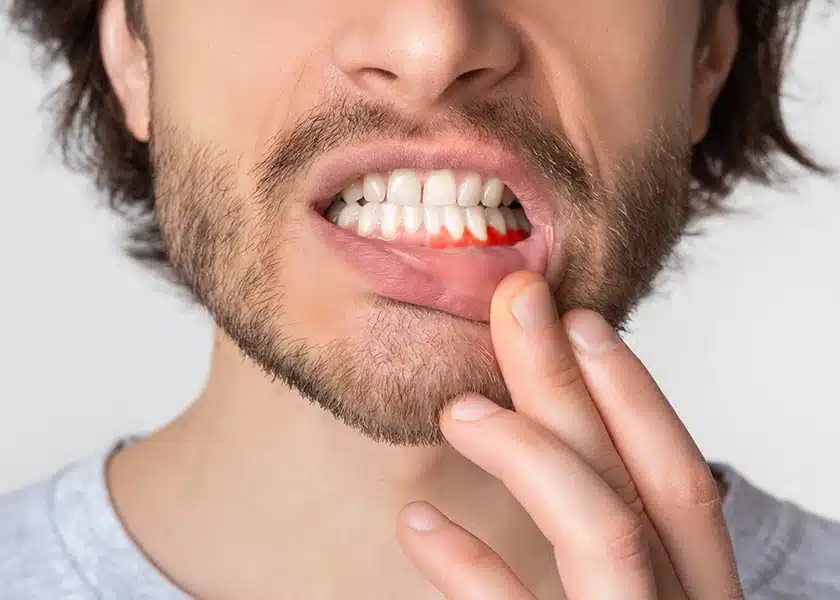
Your oral health greatly influences your overall well-being. Gum disease and severe tooth decay, which may necessitate root canal treatment, are among the issues that can arise and require specialized care.
At Diamond Dental, we often hear, “Can you get a root canal if you have gum disease?” The answer is yes. In this article titled “Gum Disease Vs Root Canal: What You Need to Know,” we aim to shed light on the relationship between gum disease and root canal treatments, helping you better understand this dental concern.
What is Gum Disease?
To determine if you’re eligible for a root canal while having gum disease, it’s crucial to understand what gum disease involves.
Gum or periodontal disease impacts the tissues surrounding and supporting your teeth. It arises mainly due to the buildup of plaque (sticky bacterial film) on your teeth. When plaque isn’t properly removed with regular oral hygiene, it can harden into tartar, triggering inflammation in the gums. It can advance to the extent of causing tooth loss.
What are the Various Stages of Gum Disease?
There are three stages of gum disease:
Gingivitis:
Gingivitis is the initial stage, characterized by red, swollen gums that can bleed while brushing or flossing.
Periodontitis:
If untreated, gingivitis can progress to periodontitis, where inflammation spreads deeper into the structures supporting the teeth. At this stage, pockets may develop between the teeth and gums, providing a space for bacteria to collect and leading to additional tissue damage.
Advanced Periodontitis:
In the advanced stage, periodontitis can cause significant harm to the bone and tissues that support the teeth, leading to tooth mobility and the risk of tooth loss.
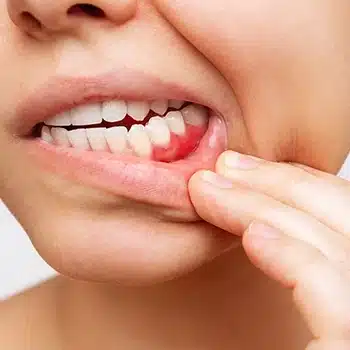
What are the Symptoms of Gum Disease?
Some common symptoms of gum disease are:
- Red, swollen, or tender gums
- Receding gums
- Persistent bad breath
- Bleeding gums, particularly during brushing or flossing
- Changes in teeth alignment
What is Root Canal Treatment?
Root canal treatment, also called endodontic therapy, is a dental procedure aimed at addressing issues within the tooth’s pulp. This pulp contains nerves, blood vessels, and connective tissue.
A root canal might be necessary when the pulp is infected or damaged due to factors like deep decay, trauma, or cracks in the tooth.
These symptoms suggest that a root canal may be necessary:
- Severe toothache while chewing or applying pressure
- Prolonged sensitivity to hot or cold temperatures
- Swollen, tender gums near the affected tooth
- Darkening or discoloration of the tooth
What does a Root Canal Procedure entail?
The root canal procedure involves several steps:
- Diagnosis: X-rays and a clinical examination are conducted to assess the extent of pulp damage.
- Anesthesia: Local anesthesia is provided to ensure the patient’s comfort throughout the procedure.
- Pulp Removal: The dentist creates an access opening to remove the infected or damaged pulp.
- Cleaning and Shaping: The root canals are carefully cleaned, shaped, and disinfected to eliminate any remaining bacteria.
- Filling: The cleared root canals are filled with a biocompatible substance, and the entry point is sealed.
- Restoration: Finally, a crown or filling is placed on the treated tooth to restore its structure and function.

What are the Factors to Consider if You Have Gum Disease and Need Root Canal Treatment?
If you’re facing gum disease and need a root canal, here are some key factors to consider:
Severity of Gum Disease:
The seriousness of your gum disease matters. While mild cases may not pose a problem for a root canal, advanced stages with significant tissue damage may need to be addressed before undergoing the procedure.
Infection Control:
If gum disease and the need for a root canal are linked to infection, controlling the spread of the infection is crucial. Dentists may prescribe antibiotics to manage the infection before proceeding with the root canal to increase the chances of success.
Tooth Stability:
The stability of the affected tooth is crucial. If gum disease has weakened the tooth’s structure, dentists will assess whether a root canal is the best option or if alternatives like tooth extraction and replacement would be more effective in the long term.
Comprehensive Evaluation:
A comprehensive evaluation of the patient’s oral health is necessary. This involves a thorough examination, often including X-rays, to determine the severity of gum disease, the condition of the affected tooth, and any existing infections. This thorough assessment allows dentists to create a personalized treatment plan tailored to the individual’s needs.
Conclusion
In the battle of Gum Disease Vs Root Canal, understanding the differences and similarities between these dental issues is crucial. While gum disease affects the supporting tissues of the teeth, root canal treatment targets issues within the tooth itself. Both conditions require prompt attention to maintain oral health and prevent further complications.
If you’re experiencing symptoms of gum disease or suspect you may need a root canal, don’t hesitate to consult with our dentist at Diamond Dental for personalized care and treatment options.
Ready to address your dental concerns and learn more about gum disease and root canal treatments? Book an appointment online with Diamond Dental in Mt. Vernon, WA, today! New patients can call (360) 512-7258, while all other callers can reach us at (360) 848-6777.
FAQ
Yes, advanced gum disease can result in damage to the tooth’s supporting structures, potentially leading to the need for a root canal.
Root canals are performed under anesthesia, so discomfort during the procedure is minimal. Some post-procedure soreness is common but manageable.
Good oral hygiene practices like regular brushing, flossing, and dental check-ups can help prevent gum disease. Timely addressing of dental issues and seeking professional care can also reduce the risk of needing a root canal.